My cortisol was still spiking at 11pm on a Tuesday. I know because I had a DUTCH test done in January 2024 — the dried urine kind that maps your full hormone metabolite picture rather than just a morning blood draw — and my free cortisol curve looked like someone had inverted the graph. Flatline in the morning when I needed it. Elevated at night when I desperately needed it gone. My naturopath called it “cortisol steal pattern with adrenal dysregulation.” I called it waking up feeling like I hadn’t slept even though the Oura ring said eight hours.
I’d been on regular coffee since I was nineteen. Two cups before 10am, occasionally a third if a deadline was brutal. It worked fine until it didn’t, and the “didn’t” came somewhere around forty-one with a level of abruptness I wasn’t prepared for. The caffeine started triggering heart palpitations by early afternoon. My sleep latency, which had always been short, stretched to forty-five minutes. I started getting that specific kind of tired that sits behind your eyes and doesn’t move.
I want to be clear upfront about something most mushroom coffee content gets wrong: the functional mushrooms in these blends aren’t there to replace caffeine’s stimulant effect. If you’re switching to Reishi and Chaga expecting a cleaner version of the same energy spike, you’re going to spend three weeks being confused and mildly disappointed before you either quit or start to actually understand what’s happening.

What Reishi Is Actually Doing at the Cellular Level in a Post-40 Body
The standard content about Reishi — Ganoderma lucidum — leads with “adaptogen” and “immune booster” and then mentions beta-glucans and triterpenes in a vague, impressionistic way. That framing isn’t wrong, it’s just incomplete in a way that makes it useless for understanding why this particular mushroom matters specifically after forty.
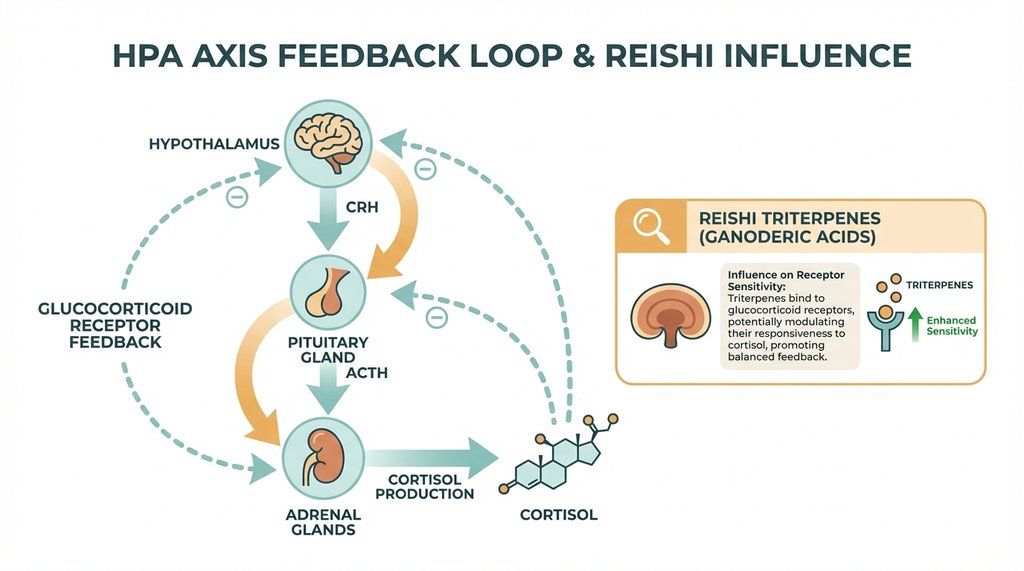
Here’s what the mechanism actually is: Reishi’s triterpenes, specifically ganoderic acids, have demonstrated inhibitory action on 5-alpha reductase. That enzyme converts testosterone to DHT and, more relevant for this conversation, is also involved in the cortisol-cortisone interconversion cycle. There’s a 2012 study in Phytomedicine (Wachtel-Galor et al.) showing immunomodulatory effects, but the more interesting work is in the area of HPA axis regulation — specifically, how Reishi polysaccharides appear to reduce overactivation of the hypothalamic-pituitary-adrenal axis under sustained psychological load.
This matters after forty because the HPA axis doesn’t break down at midlife — it dysregulates. The feedback loop that’s supposed to turn off cortisol production gets sluggish. You keep producing stress hormones longer after a stressor than you did at thirty. Reishi doesn’t suppress cortisol directly. It seems to support the sensitivity of the feedback mechanism — specifically the glucocorticoid receptor downregulation problem that happens when your receptors have been overexposed for two decades of modern life.
I noticed this most clearly not in my energy levels but in my sleep architecture. Two weeks into daily Reishi (I was using a dual-extraction product standardized to at least 15% polysaccharides and 4% triterpenes — the ratio matters, and most cheap products fail on the triterpene side), my Oura deep sleep stage increased from an average of 47 minutes to 71 minutes over the same fourteen-day tracking window. My HRV went from a baseline of 38ms to 52ms. That’s not dramatic by athlete standards, but for a 43-year-old who’d been chronically sleep-deprived, it was the difference between functional and not.
The catch: Reishi does almost nothing if you take it in the morning. This is where I made a mistake for the first six weeks. I was putting it in my morning mushroom coffee blend and wondering why I felt nothing distinctive. Reishi’s calming, cortisol-modulating effects work better taken in the evening, or split between morning and evening. When I moved my primary dose to a standalone evening tea — still getting a small amount in my morning blend, but concentrating the dose later — the sleep improvement appeared within about ten days.
Chaga’s Immune Effect Is Not What You Think It Is When You’re 40
Chaga (Inonotus obliquus) is marketed almost exclusively as an antioxidant play. The ORAC value gets cited. Melanin content comes up. This framing is partly accurate and almost entirely misses why it’s relevant to midlife immune function.
After forty, the immune issue isn’t primarily that you’re getting sick more often — though that may happen. The more insidious problem is inflammaging: the low-grade, systemic, chronic inflammatory baseline that creeps up through your thirties and forties because your innate immune system starts misfiring. Senescent cells accumulate. They release pro-inflammatory cytokines (the SASP — senescence-associated secretory phenotype) even when there’s no pathogen present. Your immune system is simultaneously becoming less responsive to actual threats and more chronically “activated” in a non-productive way.
Chaga’s beta-glucans, specifically the (1→3)(1→6)-β-D-glucans, appear to act as biological response modifiers at the level of macrophage activation. The research here is mostly in vitro and animal models — I’m not going to overstate the human clinical evidence because it’s thin. But the mechanism makes biological sense: these compounds bind to dectin-1 receptors on macrophages and dendritic cells, priming them for more accurate threat response without triggering the kind of nonspecific inflammatory cascade that characterizes inflammaging.
What I actually noticed with Chaga was less about obvious immune “strength” and more about inflammation markers. I had a CRP test in March 2024 showing 1.8 mg/L. After four months of consistent Chaga (roughly 1.5-2g daily, hot water extracted), a follow-up showed 0.9 mg/L. My GP was mildly interested but non-committal. I’m not attributing this entirely to Chaga — I also reduced processed food intake and started zone 2 cardio in that window. But the combination is worth noting, especially since the zone 2 alone should have been sufficient to move CRP in that direction, and mine had been resistant to movement for about three years despite lifestyle changes.

The sourcing issue with Chaga is genuinely serious and most content glosses over it. Chaga grown on birch trees in Siberia or the northern boreal forests has substantially different phytochemical profiles than lab-cultivated Chaga. The betulinic acid content — which is one of the compounds most associated with the anti-inflammatory activity — comes from the birch host. Lab-grown mycelium on grain substrate doesn’t have it. I went through two brands before I found one that could provide a COA showing betulinic acid content and confirming wild-harvested, birch-sourced material. This is not a minor point. It’s roughly equivalent to comparing an authentic Ashwagandha KSM-66 extract to grocery store ashwagandha powder — technically the same plant, practically a different product.
The Caffeine Reduction Issue Nobody Explains Properly
Most mushroom coffee blends cut caffeine significantly. A standard cup of regular coffee runs 95-100mg. Most mushroom coffee blends using half-caff or robusta-arabica cuts come in at 40-60mg per serving. Some are as low as 25mg.
The standard line is “you won’t feel the difference because the mushrooms provide sustained energy.” This is not what happens. What happens is that you feel the difference for the first two to three weeks, and it’s uncomfortable. I had a four-day headache starting on day two that I was not prepared for, despite having read that caffeine withdrawal could occur. I was only dropping from roughly 180mg daily to 50mg — a 72% reduction — and I felt it.
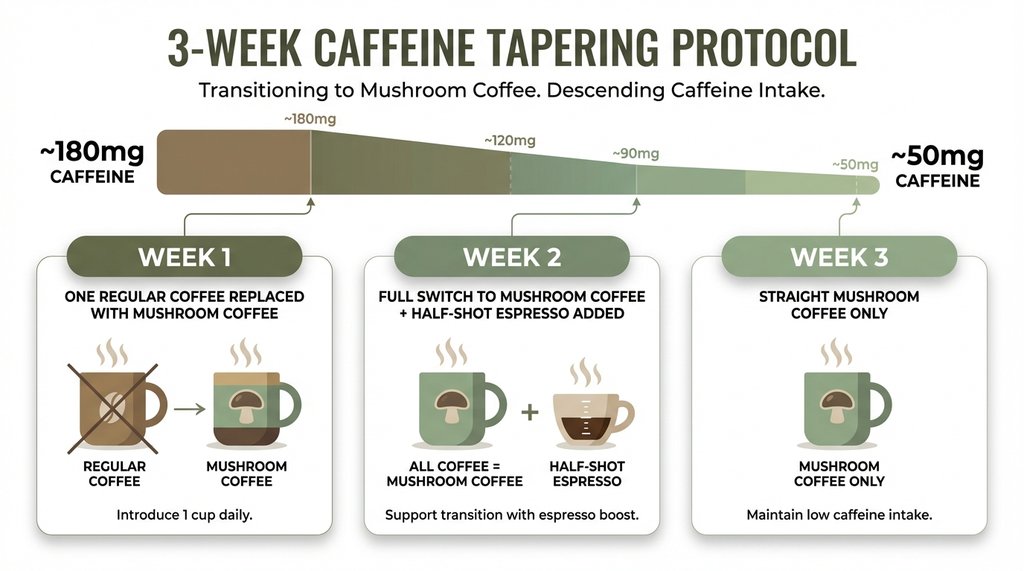
The correct protocol, which I wish someone had told me before I white-knuckled through those four days: taper over two to three weeks rather than switching directly. Week one, replace one of your two daily coffees with mushroom coffee. Week two, switch fully but add a half-shot of espresso to your mushroom coffee to keep yourself at maybe 70% of your previous caffeine load. Week three, drop to straight mushroom coffee. By that point, the mushroom compounds have had time to start working on whatever underlying fatigue you’re carrying, and the caffeine reduction feels less brutal.
I also found — and this is not a widely discussed issue — that switching abruptly made it genuinely difficult to assess whether the mushroom compounds were doing anything. I felt worse for the first ten days of my direct switch, which meant I almost abandoned the experiment before the Reishi had had any meaningful time to affect my sleep or HPA axis function. If you’re doing your own experiment here, control for caffeine withdrawal as a confound. Otherwise you’ll make the wrong conclusion.
The Hormonal Fatigue Piece Is Actually About Mitochondria, Not Hormones
Here’s the non-consensus view: “hormonal fatigue” in perimenopause and andropause is largely a downstream consequence of mitochondrial dysfunction, not simply a hormone deficiency. The hormones — declining estrogen, declining testosterone, disrupted progesterone cycles — are affecting energy at the cellular level by reducing mitochondrial biogenesis and increasing reactive oxygen species production. The fatigue isn’t primarily “you need more hormones.” It’s “your mitochondria are running less efficiently and your cells have less ATP output.”
This is why functional mushrooms can play a meaningful adjunctive role even for people who are on HRT or TRT. They’re not competing with hormonal therapies — they’re addressing a different level of the same problem. Reishi has demonstrated upregulation of Nrf2 pathway activity in multiple studies, which is the master regulator of antioxidant response in cells. Chaga’s melanin complex has direct free radical scavenging activity in mitochondria-dense tissues. You’re not replacing declining hormones. You’re reducing the oxidative damage burden that declining hormones are partly failing to protect against.
The practical implication: if you’re on HRT and still experiencing fatigue, the answer might not be adjusting your HRT dose. It might be addressing the mitochondrial substrate that the HRT alone can’t fix. This is not a reason to avoid HRT — the evidence for estrogen in particular on bone density, cardiovascular protection, and cognitive function after menopause is genuinely strong. It’s a reason to think about these interventions as operating on different axes.
What Actually Doesn’t Work
The Lion’s Mane-heavy blends marketed for cognitive function and “brain fog” in midlife are, in my experience and in my reading of the research, solving for the wrong problem when fatigue is the primary complaint. Lion’s Mane is genuinely interesting for NGF stimulation and potential neuroprotective effects. But if you’re forty-five and exhausted, your primary issue is usually not nerve growth factor — it’s cortisol dysregulation, inflammaging, and mitochondrial output. Reaching for Lion’s Mane first is like treating a cardiovascular issue with a nootropic. It’s not harmful, it’s just not targeted.
I spent three months on a Lion’s Mane-forward blend before I switched to a Reishi-and-Chaga-primary formula. The cognitive clarity effect from Lion’s Mane is real, but it’s subtle and hard to distinguish from placebo without tracking. The sleep and recovery effects from Reishi are less subtle. The CRP movement I eventually got with Chaga is measurable. If you’re early in this experiment and have limited budget, go Reishi and Chaga first, Lion’s Mane second.
The other thing that doesn’t work: products standardized only for polysaccharide content with no triterpene percentage listed for Reishi. Beta-glucans are easier and cheaper to cultivate. Triterpenes require actual fruiting body and specific extraction conditions. A product advertising “30% polysaccharides” with no triterpene data is almost certainly mycelium-on-grain-dominated, and the triterpenes are the fraction most associated with the cortisol-modulating and liver-supporting mechanisms. I spent about $180 on two products that were essentially expensive fiber supplements before I learned to look for that COA detail.

The Realistic Timeline
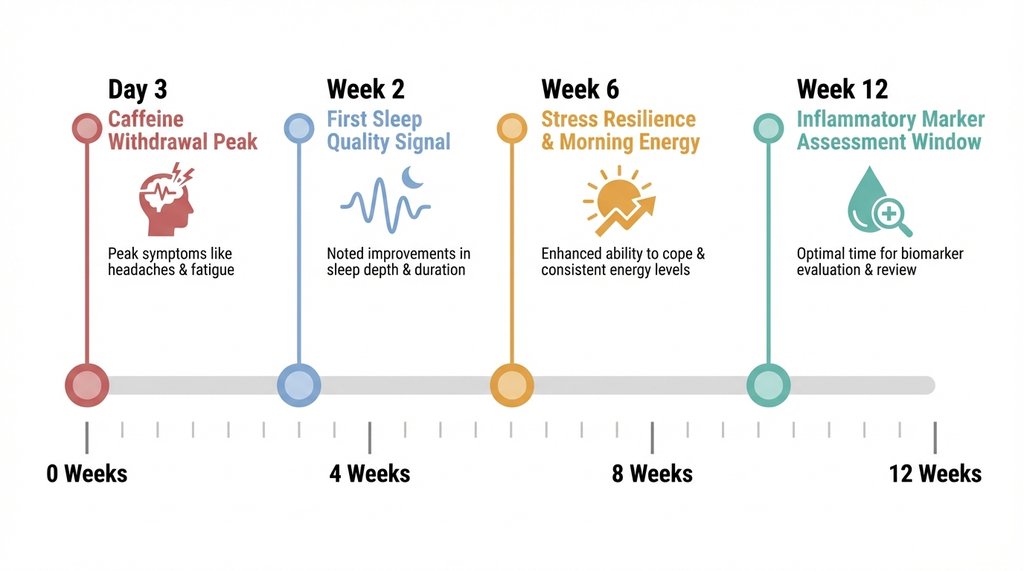
Three days: Nothing. Possibly caffeine-related headache if you switched directly.
Two weeks: Sleep quality may begin to shift if Reishi dose and timing are right. This is the most reliable early signal.
Six weeks: Some people notice improved morning energy and better stress resilience. My own experience was less linear — I had a good week three followed by a frustrating week four where I noticed almost nothing.
Three months: This is where the immune and inflammatory markers become assessable if you get bloodwork. CRP, ferritin (as an inflammatory marker, not just iron status), and if you can get it, a cytokine panel.
The people who give up at four weeks are doing so right before the window where the effects become consistent and distinguishable from background noise. That timing, I suspect, is not coincidental — it matches the point where caffeine’s absence stops being the dominant variable and the mushroom compounds would start becoming perceptible.